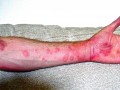
Tick Bites, Meat Allergies, and Chronic Urticaria
The rising incidence of tick-bite induced meat allergies may account for cases of previously unexplained (“idiopathic”) persistent hives among children.

The rising incidence of tick-bite induced meat allergies may account for cases of previously unexplained (“idiopathic”) persistent hives among children.

Our immune response against a foreign molecule present in animal products may play a role in some allergic, autoimmune, and inflammatory disorders. This reaction is thought to underlie tick bite-triggered meat allergies.

Used in about eight million pounds of meat every year in the United States, the “meat glue” enzyme, transglutaminase, has potential food safety and allergy implications.
The yellow pigment curcumin in the spice turmeric may work as well as, or better than, anti-inflammatory drugs and painkillers for the treatment of knee osteoarthritis.

Randomized controlled trial comparing the safety and efficacy of drugs versus curcumin, the yellow pigment in the spice turmeric, for the treatment of autoimmune inflammatory rheumatoid arthritis.

An elegant experiment is described in which the blood of those eating different types of spices—such as cloves, ginger, rosemary, and turmeric—is tested for anti-inflammatory capacity.

A plant-based diet may not only be the safest treatment for multiple sclerosis; it may also be the most effective.

A higher rate of cancer deaths among those that handle and process meat is attributed to infection with viruses, and chronic exposure to animal proteins.

Dr. Greger has scoured the world’s scholarly literature on clinical nutrition, and developed this brand-new live presentation on the latest in cutting-edge research on how a healthy diet can affect some of our most common medical conditions.

Cooked white mushroom consumption stimulates antibody production, while potentially still playing an anti-inflammatory role.

An independent review of the effects of açaí berries was recently published, including studies on immune function, arthritis, and metabolic parameters.
Plant-based diets appear to decrease inflammation via a variety of mechanisms—including boosting our adrenal gland function, due to the consumption of potassium rich foods.
Plant-based diets may help rheumatoid arthritis by decreasing exposure to an inflammatory compound found in animal products.

Plant-based diets may be protective against multiple sclerosis because IGF-1 can prevent our immune system from eliminating autoimmune cells.

We may have a billion different types of antibody-releasing cells in our immune system, such that each recognizes a different molecular signature.
Because certain tumors such as breast cancers thrive in settings of low-grade inflammation, our immune response can sometimes facilitate tumor growth.

This week Consumer Reports released a study showing the majority of retail pork tested was contaminated with antibiotic-resistant strains of the foodborne bacteria Yersinia enterocolitica.

Meat (including fish), cheese, and animal protein intake in general have been associated with an increased risk of inflammatory bowel disease (IBD). In the meantime, plant-based diets may not only help prevent such conditions, but treat them as well, resulting in the longest recorded remission rates for Crohn’s disease.
A neuropathic strain of the fecal bacteria Campylobacter, found in poultry, can trigger Guillain-Barré syndrome, a rapid and life-threatening paralysis.

Poultry workers exhibit an excess of a wide range of diseases, from thyroid conditions to schizophrenia, and autoimmune neurological disorders, such as myasthenia gravis. This may be due to exposure to viruses present in chickens and turkeys.

Arachidonic acid may play a role in cancer, asthma, inflammatory bowel disease, rheumatoid arthritis, and other autoimmune disorders.