
Side Effects of Resveratrol Supplements
Resveratrol supplements may blunt some of the positive effects of exercise training.
Topic summary contributed by volunteer(s): Lindey
Ulcerative colitis (UC), like Crohn’s disease, is an inflammatory bowel disease (IBD), an autoimmune condition in which the immune system attacks the intestines. It is typically debilitating, chronic, and recurring; there is no cure. Sufferers are often put on prescription drugs, and some undergo surgery to have segments of their intestines removed. Traditional drugs come with side effects like nausea, vomiting, headaches, rash, fever, and inflammation of the liver, pancreas, and kidneys, as well as lowered immune function and fertility.
Studies suggest that UC and other IBDs may start at a very early age. Babies fed formula rather than breast milk may have a higher risk of developing the disease. A diet high in animal protein seems to increase the risk as well, possibly due to blood components in meat, carcinogens created by cooking muscle, chemicals in processed meat, pro-inflammatory arachidonic acid and iron, harmful bacteria causing inflammation, or even the antibiotics in meat interfering with gut flora.
An animal-based diet may trigger UC by causing enzymes in the intestines to produce a harmful gas called hydrogen sulfide, which can interfere with the body’s utilization of fiber and can damage DNA. Fiber is used by our good bacteria to produce a beneficial compound called butyrate, which can reverse the adverse effect of sulfide. Fiber also helps maintain the intestinal barrier function and decrease inflammation in the colon. One study showed that women who consumed high amounts of fiber had a 40% reduced risk of IBD.
The standard American diet may have five or six times more sulfur than a diet centered on unprocessed plant foods. Sufferers of UC in remission have a higher risk of relapse with consumption of meat and alcohol, both rich sources of sulfur. Sulfur-containing amino acids are also found in dairy, eggs, and even dried fruit. Choosing organic products helps eliminates the intake of sulfur. Cabbage family vegetables naturally have some sulfur compounds, but they are not associated with elevated UC risk.
Processed foods contain ingredients that may facilitate the invasion of bacteria into the wall of the intestine, which can trigger an attack. These ingredients include polysorbate 80 (found commonly in ice cream, Crisco, Cool Whip, condiments, and cottage cheese); titanium dioxide (a whitening/brightening pigment); maltodextrin (found in Splenda, snack foods, salad dressings, and fiber supplements); and sucralose, which has been shown to increase IBD rates up to twelvefold. The good news is that after stopping consumption, the original balance of gut bacteria may be restored within weeks.
Studies have shown that drinking wheatgrass juice or ingesting curcumin and oat bran appear effective and safe to decrease symptoms of disease activity and prevent relapse. Also, eliminating dairy may help roughly one in five sufferers. Cruciferous vegetables such as broccoli, cauliflower, and cabbage are essential for sustaining colon health. But the best therapy (and prevention) is a whole food plant-based diet.
For substantiation of any statements of fact from the peer-reviewed medical literature, please see the associated videos below.
Image Credit: Pixabay. This image has been modified.

Resveratrol supplements may blunt some of the positive effects of exercise training.

Resveratrol appears to triple the rate of age-related brain shrinkage.

A study using sham acupuncture underscores the necessity of controlling for expectancy effects.
I go over randomized, controlled trials and case reports of stool transplants for various clinical conditions.

Even though cannabis smoking may help with IBD symptoms in the short-term, it may make the long-term prognosis worse.

Switching to a plant-based diet has been shown to achieve far better outcomes than those reported on conventional treatments in both active and quiescent stages in both Crohn’s disease and ulcerative colitis.

Plant-based diets can be 98 percent effective in keeping ulcerative colitis patients in remission, blowing away other treatments.

Eating a diet filled with animal products can disrupt your microbiome faster than taking an antibiotic.

What’s the best type of pots and pans to use?

Is the exaggerated reaction of many Crohn’s disease patients to baker’s, brewer’s, and nutritional yeast just a consequence of their inflamed leaky gut, or might the yeast be a contributing cause?

Vitamin D supplements were put to the test for Crohn’s disease.

A randomized, double-blind, placebo-controlled trial found wheatgrass juice to be safe and effective in the treatment of an inflammatory bowel disease.

A double-blind, placebo-controlled trial found a dramatic effect of the anti-inflammatory spice pigment curcumin against inflammatory bowel disease.

What effect do artificial sweeteners such as sucralose (Splenda), saccharin (Sweet & Low), aspartame (Nutrasweet), and acesulfame K (Sweet One) have on our gut bacteria?
What happens to our gut flora microbiome when we’re on plant-based versus animal-based diets?

If the avoidance of sulfur-rich proteins and food additives can help prevent inflammatory bowel disease, might similar dietary changes help prevent relapses of ulcerative colitis?
Sulfur dioxide preservatives in dried fruit, sulfites in wine, and the putrefaction of undigested animal protein in the colon can release hydrogen sulfide, the rotten egg gas associated with inflammatory bowel disease.
The toxic rotten egg gas hydrogen sulfide may explain why animal protein is associated with inflammatory bowel disease.
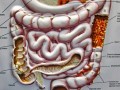
Diets centered around whole plant foods may help prevent Crohn’s disease through the benefits of fiber on the maintenance of intestinal barrier function and the avoidance of certain processed food additives such as polysorbate 80.

For more than 30 years, the medical profession has debated the existence of an intolerance to the wheat protein, gluten, unrelated to allergy or celiac disease. What is the evidence pro and con?

There is a receptor in our intestines activated by phytonutrients in cruciferous vegetables that boosts immune function (the aryl hydrocarbon [Ah] receptor).

People eating conventional diets may ingest a trillion microparticles of the food-whitening additive, titanium dioxide, every day. What implication might this have for inflammation in the gut?
Because certain tumors such as breast cancers thrive in settings of low-grade inflammation, our immune response can sometimes facilitate tumor growth.

Exclusive breastfeeding for a full six months may, ironically, improve our children’s taste for vegetables—whereas children fed formula grow up with increased rates of inflammatory diseases such as asthma, cancer, and diabetes.

Arachidonic acid may play a role in cancer, asthma, inflammatory bowel disease, rheumatoid arthritis, and other autoimmune disorders.