
Brain Health
Topic summary contributed by volunteer(s): Charlie
Lifestyle changes, including a healthy diet, physical exercise, and mental exercise could play an important role in the prevention of Alzheimer’s disease (see also here). A Mediterranean diet may not only reduce risk of Alzheimer’s, but may also reduce mortality from the disease. Different fruits and vegetables appear to support different cognitive domains of the brain, so both variety and quantity in the diet are important. Greater fruit and vegetable consumption has been linked with lower rates of dementia and Alzheimer’s disease. The consumption of blueberries and strawberries is associated with delayed cognitive aging by as much as 2.5 years. Ellagic acid may play a role in the ability of berries to prevent age related cognitive decline, but its absorption is blocked by dairy.
The relationship between tofu and dementia may be related to formaldehyde contamination. Apple juice did not appear to increase cognitive performance in Alzheimer’s patients, even though in a petri dish, apple juice and ginger appeared to improve nerve cell survival. However, it has been found that those who drink fruit and vegetable juices had a 76% lower risk of developing Alzheimer’s, possibly due to phytonutrient content. Saffron, when compared to Aricept, a leading drug in the treatment of Alzheimer’s, was found to work just as well without the side effects (see also here). While populations eating more turmeric have a lower incidence of Alzheimer’s, this may be due to their lower consumption of meat, which is also beneficial for Parkinson’s disease. However, turmeric, but not curcumin supplements, was found to alleviate Alzheimer patients’ symptoms. Coffee may also reduce the risk of Parkinson’s and Alzheimer’s. Conversely, there is little evidence that coconut oil helps with Alzheimer’s disease. Aluminum is added to processed cheese and may be related to neurodegenerative diseases such as Alzheimer’s. Similarly, iron accumulation in the brain is being increasingly linked to neurological diseases such as Alzheimer’s, glycotoxins (found mostly in chicken) may increase the risk of developing Alzheimer’s disease, and BMAA, a neurotoxin found in seafood may also be linked with higher rates of neurodegenerative disease. Moreover, there’s been a recommendation that people with a family history of neurodegenerative diseases should avoid milk. Toxic waste in the food supply may help explain the link between dairy consumption and Parkinson’s disease (see also here). Skim milk has been found to have especially high levels of hormones. There may be a simple, cheap, non-invasive test for detection of Alzheimer’s disease.
Consumption of methyl mercury can result in microcephaly, impaired cognition, and delayed brain-nerve communication in fetuses, infants, and children. Mercury contamination has also been linked to lower IQs and brain damage in the children of mothers who ingest mercury while pregnant. Women may want to avoid polluted fish consumption for a year before they get pregnant in addition to just during pregnancy. Methyl mercury is found in tuna and fish (see here, here and here). Ayurvedic medications have also been found to be contaminated with mercury and lead. Arsenic is fed to chickens and may be related to neuropathy as well as neurocognitive deficits in children. Getting bitewing or panoramic X-rays at the dentist may be associated with an increased risk of meningioma, the most common type of brain tumor. Dehydration may impair cognitive functions.
Pork tapeworms larvae invading the brain is one of the most common causes of epilepsy (see also here), and may present as migraines or chronic tension headaches. The brain parasite toxoplasma is found in lambs; 10% of Americans are currently infected with this parasite. There are also migratory skin worms from sushi consumption that may get into the brain. Neurotoxic chemicals in chicken, including beta-carboline alkaloids, may also explain the link between meat consumption and the common neurological disorder essential tremor. Similarly, domoic acid, found in seafood, has been found to cause an unusual form of amnesia.
Aspirin naturally found in plants may explain the presence of aspirin in the bloodstream of vegetarians. The omega-3 fatty acids our brain needs for optimal health (both long and short chain) can be obtained from plant sources. Blue-green algae can produce neurotoxins and should be avoided. Cognitive deficits may be an early sign of B12 deficiency, which is more frequent in vegans and vegetarians than omnivores (see also here).
For substantiation of any statements of fact from the peer-reviewed medical literature, please see the associated videos below.
Image Credit: Pixabay. This image has been modified.
Popular Videos for Brain Health


Do Lutein Supplements Help with Brain Function?
Avocados, greens, and lutein and zeaxanthin supplements are put to the test for improving cognitive...
Brain-Healthy Foods to Fight Aging
What is the best source of lutein, the primary carotenoid antioxidant in the brain?
Fighting Autism Brain Inflammation with Food
One food may be able to combat all four purported causal factors of autism: synaptic...
Cell Phone Brain Tumor Risk?
What does the world’s leading authority on carcinogens have to say about mobile phones?
Does Cell Phone Radiation Cause Cancer?
Do mobile phones cause brain tumors? Whenever a trillion-dollar industry is involved—whether it’s Big Food,...
Saffron vs. Memantine (Namenda) for Alzheimer’s
The spice saffron is pitted head-to-head against the leading drug for severe Alzheimer’s disease.
Higher Blood Pressure May Lead to Brain Shrinkage
Having hypertension in midlife (ages 40 through 60) is associated with elevated risk of cognitive...
Benefits of Rosemary for Brain Function
A half teaspoon of dried rosemary can improve cognitive function.
Should Vegans Take DHA to Preserve Brain Function?
Learn why I recommend 250mg a day of a pollutant-free source of long-chain omega-3 fatty...
Should We Take DHA Supplements to Boost Brain Function?
Overt omega-3 deficiency is rare, but do short-term experiments on cognitive function suggest there might...
Alzheimer’s May Start Decades Before Diagnosis
Neurodegenerative brain changes begin by middle age, underscoring the need for lifelong preventive brain maintenance.
Alzheimer’s and Atherosclerosis of the Brain
Lack of adequate blood flow to the brain due to clogging of cerebral arteries may...
Aspartame and the Brain
The reason artificially sweetened beverages have been associated with depression may be because of psychological...
Preventing Brain Loss with B Vitamins?
One week on a plant-based diet can significantly drop blood levels of homocysteine, a toxin...
Preventing Alzheimer’s Disease with Diet
The role of the Mediterranean diet in preventing and treating dementia.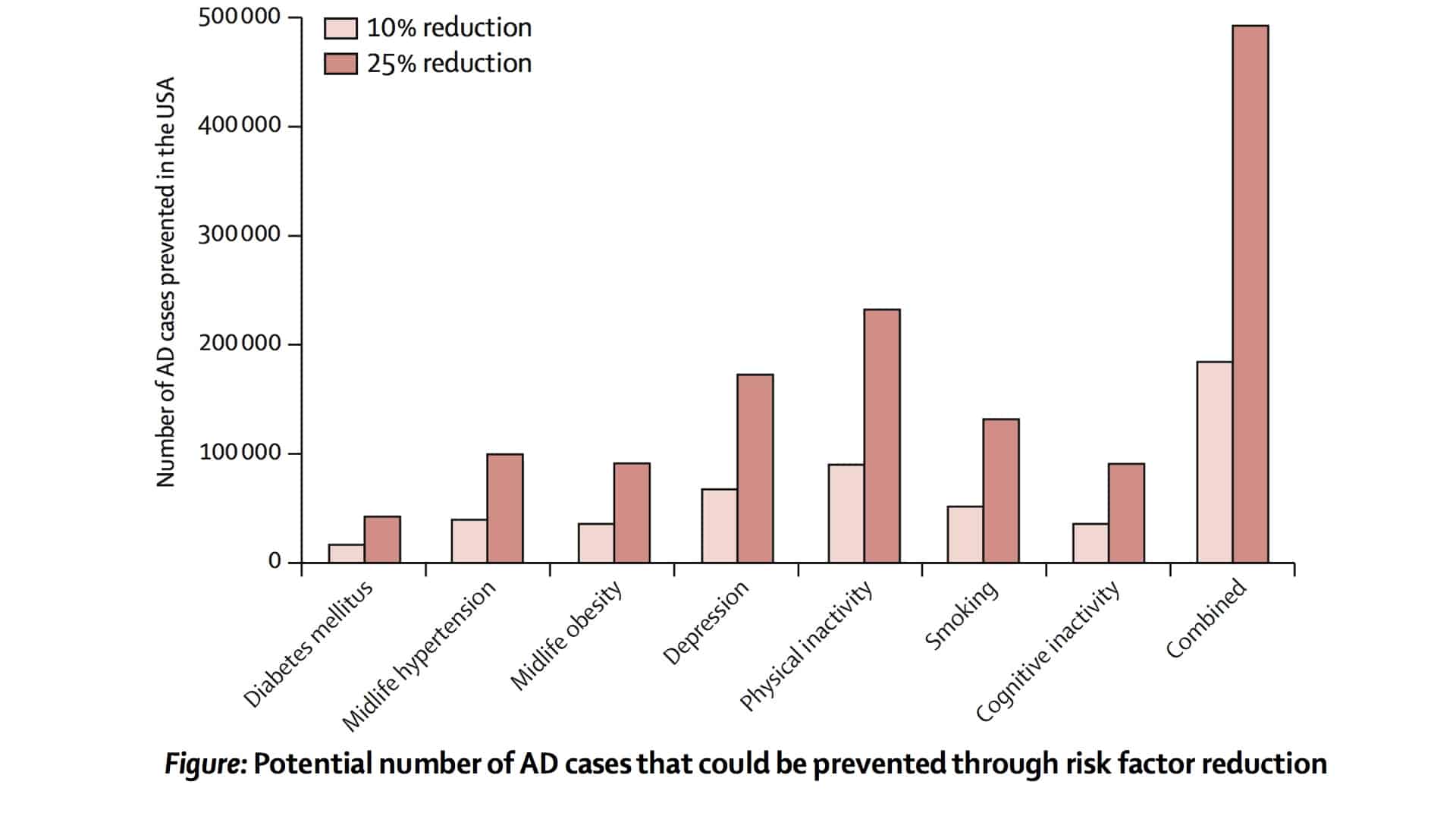
Preventing Alzheimer’s with Lifestyle Changes
Lifestyle changes could potentially prevent hundreds of thousands of cases of Alzheimer’s disease every year...
Alzheimer’s Disease: Grain Brain or Meathead?
Grain consumption appears strongly protective against Alzheimer’s disease, whereas animal fat intake has been linked...
How to Slow Brain Aging by Two Years
The consumption of blueberries and strawberries is associated with delayed cognitive aging by as much...
Mercury vs. Omega-3s for Brain Development
Risk/benefit analysis of 33 fish species contrasts the brain-boosting effects of DHA with the brain-damaging...All Videos for Brain Health
-

The Side Effects of Statins: Are They Worth It?
When statin-“intolerant” patients are challenged blindly, how many are really suffering muscle side effects?
-

The Benefits of Black and Green Teas for Brain Waves
Of all the plants in the world, why has the tea plant become the most popular beverage in the world?
-

Do Not Eat Pawpaws
Pawpaw fruits, like soursop, guanabana, sweetsop, sugar apple, cherimoya, and custard apple, contain neurotoxins that may cause a neurodegenerative disease.
-

Risks of NAD+ Boosting Supplements
Particular caution should be used for NAD+-boosting supplements by those with cancer, a personal or strong family history of cancer and perhaps also by those with inflammatory disorders and certain active infections.
-

Can NAD+ Boosters Increase Lifespan and Healthspan?
The effects of NAD+ boosters on aged rodents have been described in the medical literature as “profound,” “dramatic,” and “remarkable,” but do they help people?
-

What Is Essential Hand Tremor and How to Prevent and Treat It
What is the role of dietary beta-carboline alkaloids in the development of the most common movement disorder?
-

Do Ashwagandha, Ginseng, and Maca Root Have Benefits for Female Sexual Dysfunction?
Which of these three works, which doesn’t, and which may be too toxic to take safely?
-

The Best Way to Boost NAD+: Supplements vs. Diet (webinar recording)
The pros and cons of all the NAD+ supplements and what are the ways to boost NAD+ naturally with diet and lifestyle?
-

The Risks and Benefits of Mild Trendelenburg Position to Reduce Body Fat
Other than a “space headache,” what might be the downsides of sleeping at a slight head-down tilt to accelerate fat loss?
-

How Much Exercise Does It Take to Improve Aging Cognitive Function?
If the relationship between exercise and dementia prevention is cause-and-effect, as much as 20 percent of Alzheimer’s disease may be attributable to physical inactivity.
-

Can Vitamin E or Selenium Supplements Prevent or Treat Alzheimer’s?
The Prevention of Alzheimer’s Disease by Vitamin E and Selenium trial randomized more than 7,500 older men to take vitamin E, selenium, both, or neither (just placebos) for five years.
-

A Testimonial from Dr. Ornish’s Alzheimer’s Progression Reversal Study
What does improving the cognition and function of Alzheimer’s patients with lifestyle medicine actually translate to in terms of human impact?
-

Can Alzheimer’s Disease Be Reversed with a Plant-Based Diet?
Dr. Dean Ornish publishes the first randomized controlled trial investigating whether a plant-based diet and lifestyle program may reverse the course of early-stage Alzheimer’s disease.
-

Dental Implant Overdentures and Cognitive Function
Chewing pressure sensations to the nerves in the jaw have neurological effects.
-

The Best Sleeping Position for Glymphatic Flow in the Brain
What can we do to prevent the decline in glymphatic brain filtration as we age?
-

How Much Sleep Is Needed for Glymphatic Flow (Brain Cleaning)?
One function of sleep is the clearance of toxic waste byproducts through a newly discovered drainage system in the brain.
-

Ginkgo Biloba as a Brain Health Supplement for Dementia
Ginkgo does not seem to play a role in preventing cognitive decline or dementia, but it may play a role in treating it.
-

Does Prevagen Really Work?
Why did the makers of Prevagen settle a class action lawsuit in 2020 with the FTC over deceptive business practices and false advertising? Is Prevagen safe?
-

Controversy Around FDA’s Approval of Biogen Alzheimer’s Drug, Aducanumab
I discuss the safety and efficacy of the newest Alzheimer’s drug treatments, aducanumab (Aduhelm) and lecanemab (Leqembi).
-

Are There Any Side Effects to Taking Creatine?
A misinterpretation of lab tests may explain concerns over kidney safety with creatine supplementation.
-

What Is Creatine? Can It Treat Sarcopenia (Muscle Loss with Age)?
When accompanied by a progressive strength-training regimen, 3 grams of creatine a day may improve muscle performance in older adults.
-

The Role of Endotoxins in Alzheimer’s and Dementia
Why can a single meal high in saturated fat impair cognition?
-

Advanced Glycation End Products (AGEs) and Cognitive Decline
AGEs may be one explanation for why those who consume meat may have up to three times the risk of developing dementia compared with vegetarians.
-

Can Vegan Fecal Transplants Lower TMAO Levels?
If the microbiome of those eating plant-based diets protects against the toxic effects of TMAO, what about swapping gut flora?
-

The Dangerous Effects of Heavy Metal Music
How might we moderate the rare but very real risk of headbanging?
-

Fasting for Post-Traumatic Brain Injury Headache
What effect do fasting and a plant-based diet have on TBI and migraines?
-

Lychee Fruit and Hypoglycin: How Many Are Too Many?
There is a toxin in lychee fruit that can be harmful, but only under certain circumstances?
-

The Effects of Obesity on Dementia, Brain Function, and Fertility
Weight loss can decrease dementia risk and improve mental performance and infertility.
-

The Efficacy and Safety of Creatine for High Homocysteine
Those on a healthy plant-based diet with elevated homocysteine levels despite taking sufficient vitamin B12 may want to consider taking a gram a day of contaminant-free creatine.
-

Should Vegetarians Take Creatine to Normalize Homocysteine?
What are the consequences of having to make your own creatine rather than relying on dietary sources?
-

How to Test for Functional Vitamin B12 Deficiency
Many doctors mistakenly rely on serum B12 levels in the blood to test for vitamin B12 deficiency.
-

Vegetarians and Stroke Risk Factors—Vitamin B12 and Homocysteine?
Not taking B12 supplements or regularly eating B12 fortified foods may explain the higher stroke risk found among vegetarians.
-

Vegetarians and Stroke Risk Factors—Animal Protein?
Might animal protein-induced increases in the cancer-promoting grown hormone IGF-1 help promote brain artery integrity?
-

Vegetarians and Stroke Risk Factors—Saturated Fat?
How can we explain the drop in stroke risk as the Japanese diet became Westernized by eating more meat and dairy?
-

Vegetarians and Stroke Risk Factors—Vegan Junk Food?
Just because you’re eating vegetarian or vegan doesn’t mean you’re eating healthy.
-

Vegetarians and Stroke Risk Factors—Omega 3s?
Does eating fish or taking fish oil supplements reduce stroke risk?
-

Vegetarians and Stroke Risk Factors—Vitamin D?
Could the apparent increased stroke risk in vegetarians be reverse causation? And what about vegetarians versus vegans?
-

Do Vegetarians Really Have Higher Stroke Risk?
The first study in history on the incidence of stroke of vegetarians and vegans suggests they may be at higher risk.
-

What Not to Eat for Stroke Prevention
What is the relationship between stroke risk and dairy, eggs, meat, and soda?
-

What to Eat for Stroke Prevention
More than 90% of stroke risk is attributable to modifiable risk factors.
